Recently, premature female triplet infants afterin vitrofertilization and embryo transfer (IVF-ET) with a gestational age of over 28 weeks, weighed from 1090 gram to2000 gram,were admitted to Department of Neonatology of the First Affiliated Hospital of Xi’an Jiaotong University (XJTU). All infants were transferred to the premature infant incubators for more than 50 days after birth and experienced many life-threatening challenges. Just as they were getting better day by day, the oldest infant was diagnosed with retinopathy of prematurity (ROP) by fundus screening examination: stage 3 ROP in zone II (OD) and stage 3 ROP in zone II with plus disease (OS), which have evolved into the threshold stage. If not intervened early, it was likely to increase the risk of blindness.
IVF-ET triplet infants with low gestational age and very-low-birth weight brought huge challenges to subsequent treatment. Pei Cheng, Director of Department of Ophthalmology discussed with Professor Liu Siwei, Attending Physician Cheng Yuhong and Zhou Xihui, Director of Department of Neonatology to choose intravitreal injection. Conventionally, for low gestational age and low-birth-weight premature infants, ocular surgery should be performed via tracheal intubation under general anesthesia, which can provide optimal conditions for airway patency, ventilation and oxygen supply and intraoperative rescue, whereas tracheal intubation will aggravate damage and harm to the infants. After comprehensive communication among the ophthalmic treatment team, Department of Anesthesia and Department of Neonatology, it was decided to complete the surgery under the induction of anesthesia via mask inhalation without intubation. However, this technique can merely yield superficial anesthesia and the pain stimulation induced by intraoperative needle insertion into the eye may provoke eyeball movement, which further increases the risk of lens damage.
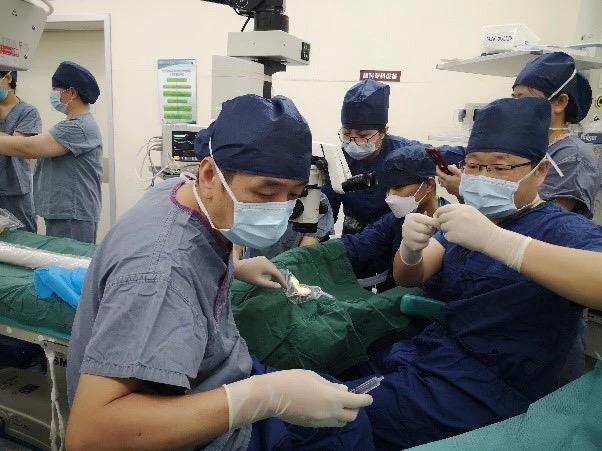
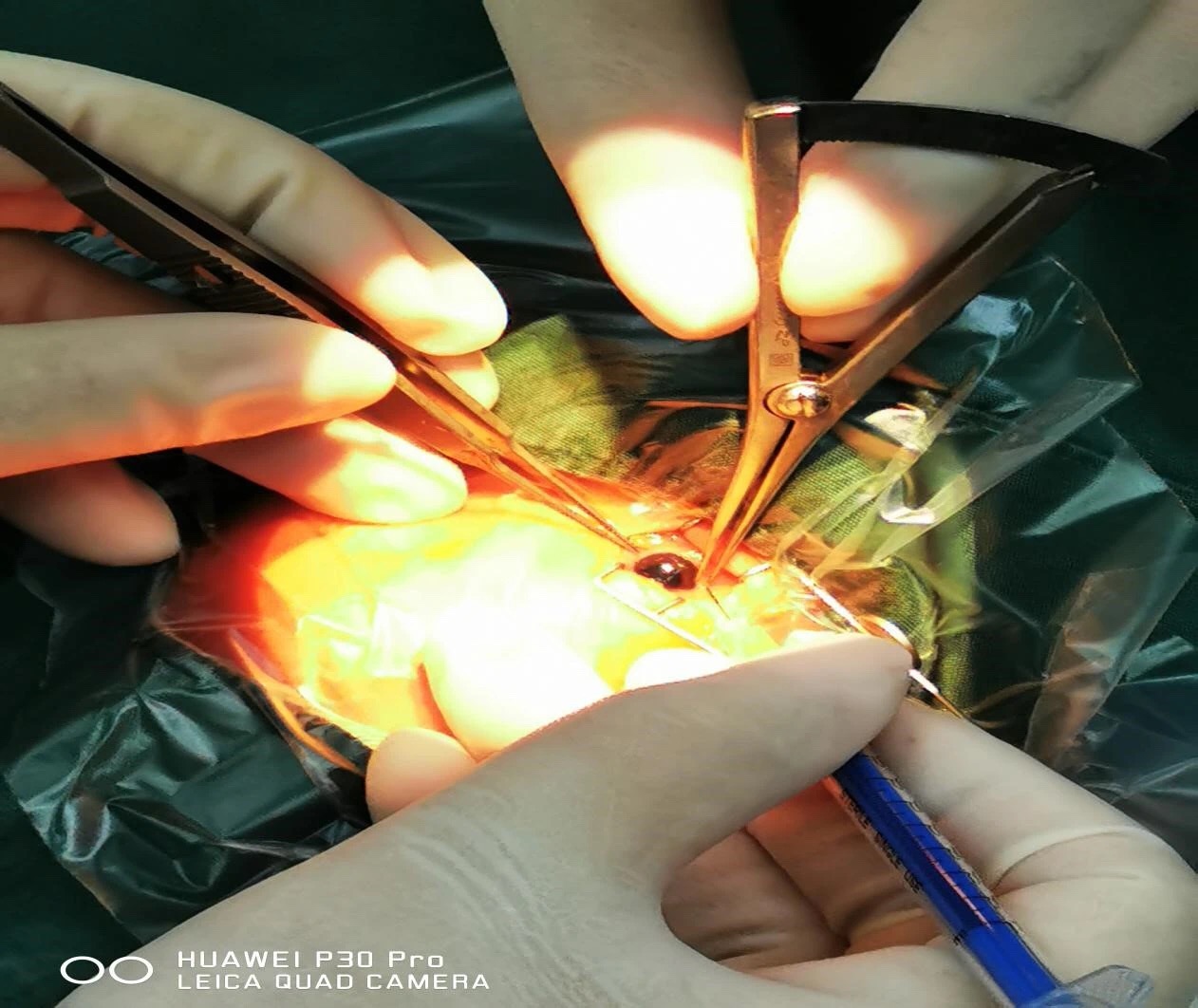
On March 17, with the assistance of Physician Tong Hua from Department of Anesthesia and Xiao Mi from Department of Neonatology, Professor Liu Siwei and Attending Physician Cheng Yuhong jointly performed intravitreal injection for this premature infant. Although the operation time was relatively short, intravitreal injection might cause lens injury and even lead to iatrogenic cataract due to the small and immature infantile eyeballs with special anatomical structures and the soft and fragile eyeball wall, which may aggravate the eyeball damage of the infant. The surgery was successfully accomplished under precise operation and collective cooperation.
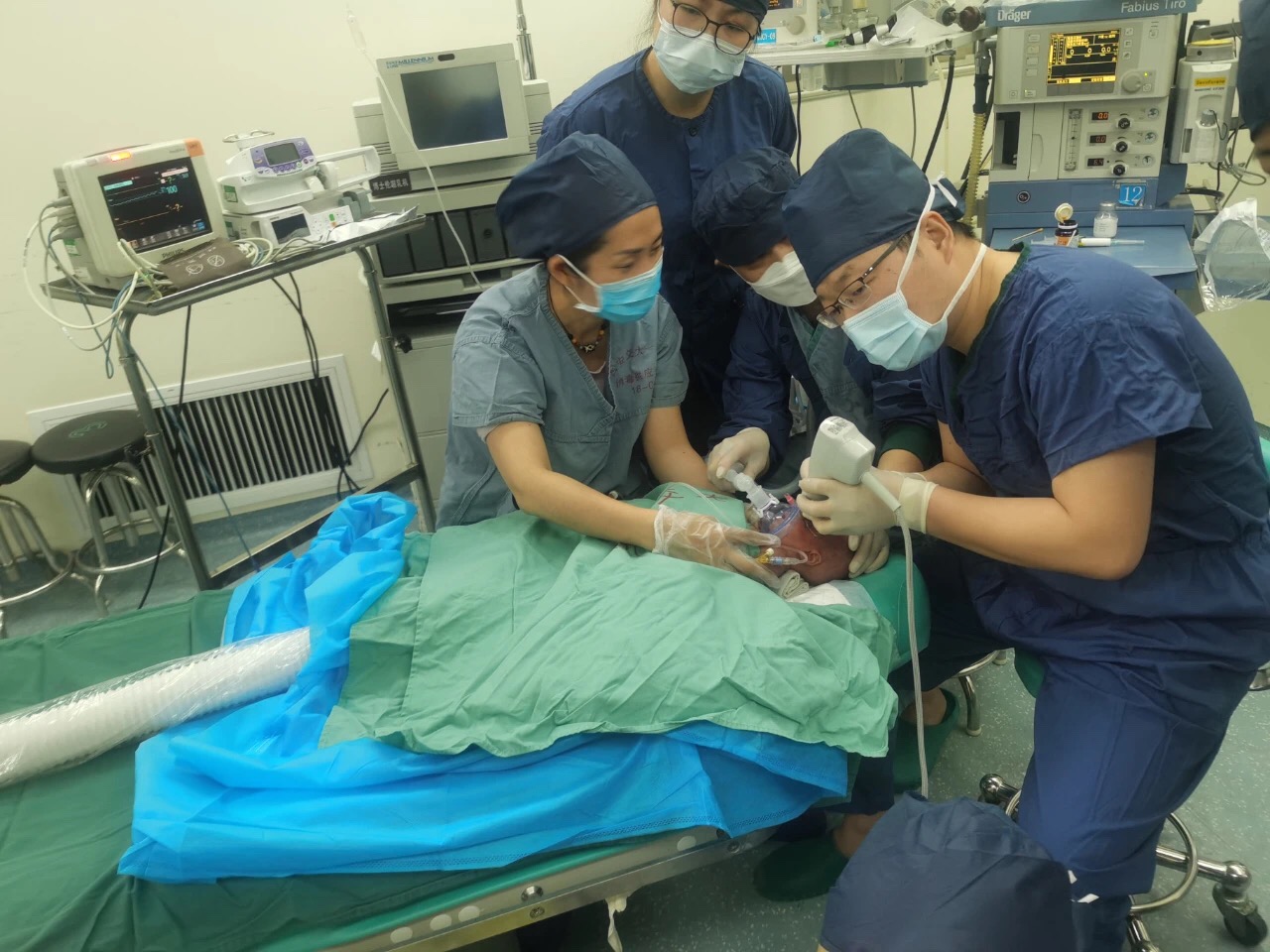
However, an unexpected incident occurring during the operation still made everyone nervous. The infant fell asleep after successful induction of inhalation anesthesia. After Professor Liu Siwei marked the location of needle insertion, Attending Physician Cheng Yuhong promptly inserted the needle according to the marked location and injected the drug into the right eye! When surgeons were prepared to start the left eye surgery, the oxygen saturation was dramatically declined and the facial skin turned purple, making everyone nervous. Physician Tong Hua immediately delivered deep anesthesia and increased the oxygen intake. Subsequently, the oxygen saturation was gradually restored to normal range and her complexion became ruddy. The left eye surgery was eventually completed. After the operation, the infant was well recovered and transferred to the neonatal ward.
On March 26, Attending Physician Cheng Yuhong delivered the first postoperative fundus reexamination for the infant. Surprisingly, the stage 3 ROP and plus lesions of bilateral eyes were significantly alleviated to stage 1 and stage 2 ROP, respectively. The retinal vessels continually grew toward peripheral fundus.
On April 1, Physician Chen Li performed the second postoperative fundus reexamination and found the severity of ROP in bilateral eyes was mitigated to stage 1 ROP and retinal vessels continued to normally grow. After timely examination and treatment by the ophthalmology team, this premature infant was temporarily prevented from the risk of blindness.
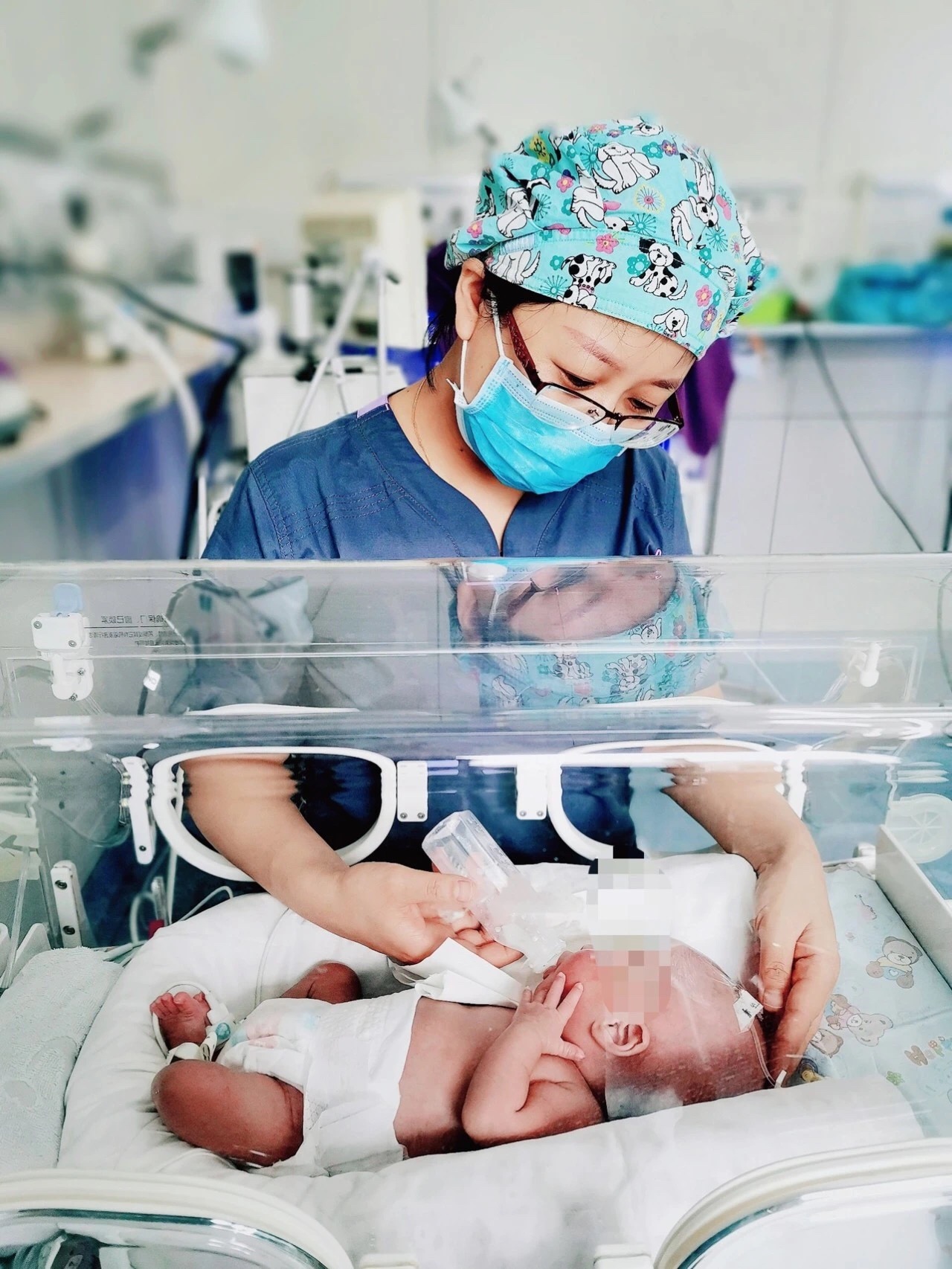
During the treatment of the oldest infant, her two little sisters also received fundus examinations. For the second oldest infant, the severity of lesions was controllable and fundus examimation was conducted weekly. No treatment was required and the regime was timely adjusted according to the severity of lesions. Fundus examination detected no pathological changes in the little sister. Intimate monitoring and reexamination were delivered until the retinal vessels developed into maturity.
Compared with laser therapy, intravitreal injection of anti-vascular endothelial growth factors (Rezumab or Conbercept) has multiple advantages in the treatment of ROP, such as less impact on retinal vascular development and preserving a larger retinal functional area, especially suitable for severe ROP in the fundal posterior polar region. After more than 10 years of ROP screening, our hospital has established a team which consists of Department of Ophthalmology and Department of Neonatology for the management of neonatal eye diseases. It features strong professional strength in ocular fundus diseases and solid skills of indirect ophthalmoscopy, which is the earliest and one of the few institutions to carry out this surgery in Shaanxi province and northwest China.