Recently, the hepatobiliary surgery team at the First Affiliated Hospital (FAH) of Xi’an Jiaotong University (XJTU), led by Associate Chief Physician Hu Liangshuo and Professor Wang Bo, published a significant research finding in International Journal of Surgery (Impact Factor: 10.3). The team pioneered the integration of near-infrared hyperspectral imaging with deep learning, establishing a novel intelligent evaluation system for donor livers in liver transplantation and providing an innovative solution to the longstanding clinical challenges in donor liver assessment. Doctoral candidate Wang Zichen is the first author, and Wang Bo and Hu Liangshuo serve as co-corresponding authors.

Currently, donor liver quality assessment in liver transplantation faces challenges such as subjectivity, invasiveness, and time consumption; the widespread use of marginal donor livers further exacerbates postoperative risks, creating an urgent clinical need for rapid, objective, and non-invasive assessment technologies. The team developed a near-infrared hyperspectral imaging system tailored to donor liver procurement surgery and, together with deep learning models, established an intelligent evaluation framework. Within the 900-1,700 nm spectral range, the system enables non-invasive spectral quantification of hepatic lipids and key inflammatory mediators such as IL-1β; the model achieved a prediction accuracy exceeding 0.9, performing markedly better than conventional methods.
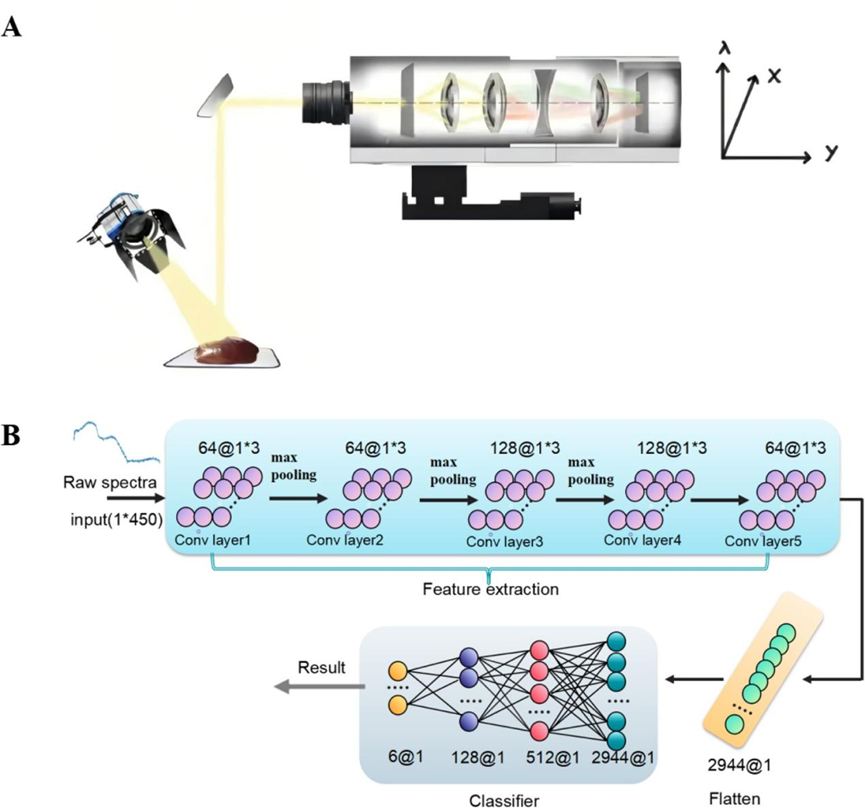
The AI model built in this study achieved a grading-and-classification accuracy of over 99% for hepatic steatosis and ischemia-reperfusion injury, and it can also predict early graft dysfunction based on spectral differences. By integrating targeted lipidomics, the team elucidated, at the molecular level, the biological basis underlying changes in spectral signals, providing new leads for targeted intervention.
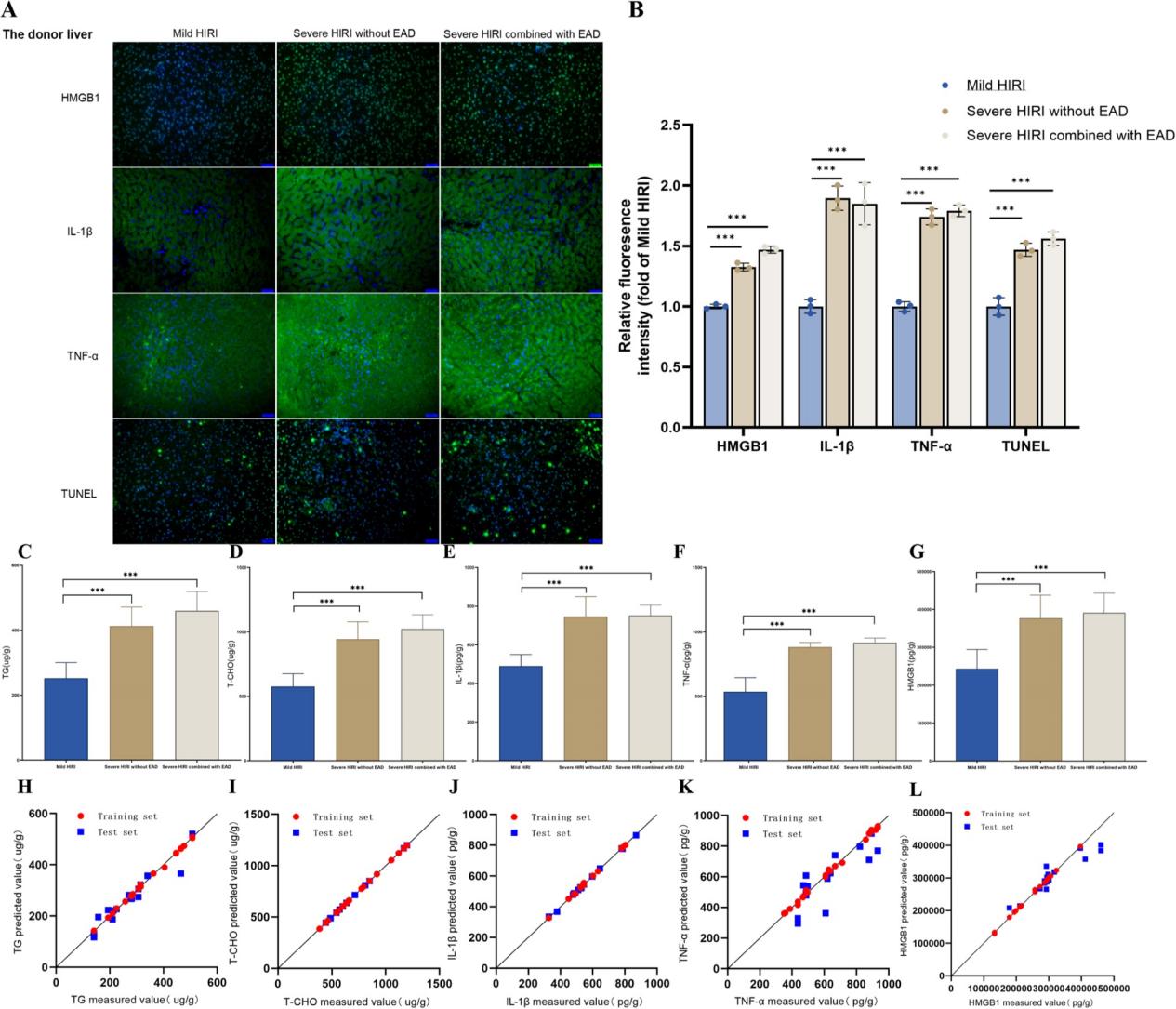
This achievement represents a breakthrough in the medical application of hyperspectral technology and carries substantial clinical translational value: it enables real-time, non-invasive, full-field intraoperative assessment and early warning of postoperative complications, and may be integrated into machine perfusion platforms in the future to optimize donor liver repair and utilization. The research was led by the FAH’s liver transplantation team and completed in collaboration with multiple universities and research institutes, serving as a model of deep integration of clinical and basic research and multidisciplinary, cross-domain collaboration, and holding major significance for improving liver transplantation success rates and expanding the donor pool.
Article Link:https://dx.doi.org/10.1097/JS9.0000000000004819